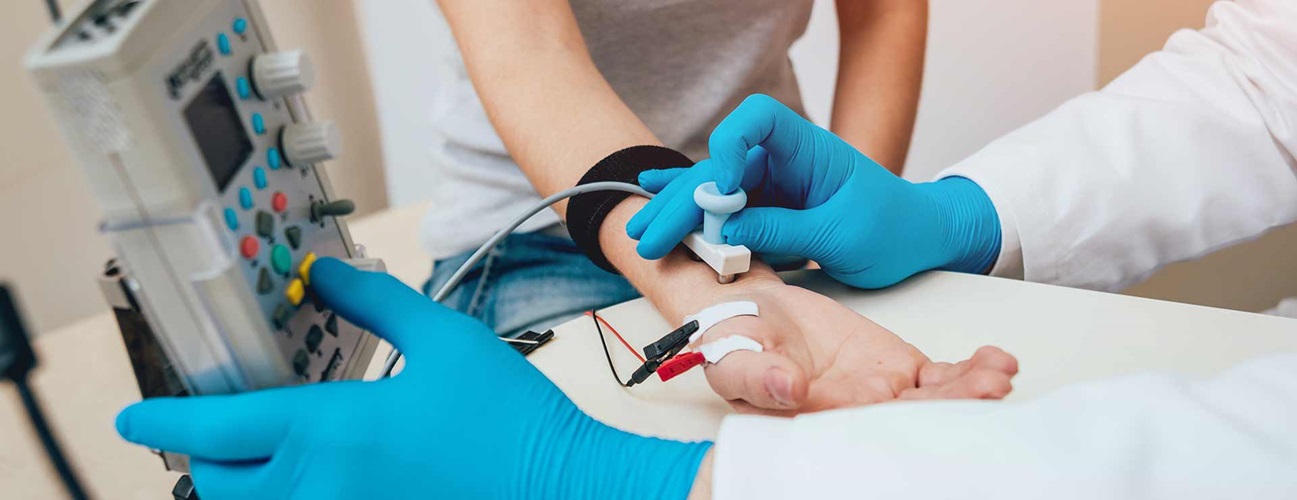
In the field of Independent Medical Examinations (IME), one important evaluation tool used is Electromyography (EMG). This test assesses the function of nerves and muscles by detecting electrical activity in the body. An EMG test involves placing small electrodes on the skin or inserting needle electrodes into muscles. It can provide valuable information to doctors in diagnosing and monitoring a range of conditions. In this article, we will explore the purpose of EMG tests in IMEs, why doctors may order them, the diseases they can detect, the level of discomfort involved, and what abnormal results may indicate. We will also specifically address EMG tests conducted on the legs. Stay tuned to unlock the link between Independent Medical Examinations and EMG.
What is an electromyography EMG test?
Electromyography (EMG) is a diagnostic test that evaluates the function of nerves and muscles. It involves the use of electrodes, which are placed on the skin or injected into muscles, to measure the electrical activity produced by muscle fibers when they contract. This test helps physicians assess the health and functionality of the nerves that control muscles and can provide valuable information about the underlying cause of muscle weakness, pain, or other related symptoms. EMG tests can be conducted on various parts of the body, including the arms, legs, neck, and back.
How are EMGs used in IMEs?
Electromyography (EMG) is occasionally used as part of Independent Medical Examinations (IMEs) to provide valuable insights into a patient’s neuromuscular function and help assess the extent of injuries or disabilities. Here’s how EMGs can be utilized in the context of IMEs:
- Objective Assessment: EMG provides objective data about a patient’s neuromuscular function. During an IME, an impartial physician or healthcare provider may use EMG to objectively evaluate the patient’s muscle and nerve health, ensuring an unbiased assessment.
- Determining Disability or Impairment: In cases where a patient is claiming disability or impairment due to a work-related injury or accident, EMG can help determine the extent of the impairment. By measuring muscle weakness, nerve damage, or abnormal electrical activity in muscles, EMG results can support or refute the patient’s claims.
- Verification of Symptoms: Some patients may report symptoms such as muscle weakness, pain, or sensory disturbances. EMG can help verify the presence and severity of these symptoms by providing quantitative data. This is particularly important when there is a discrepancy between reported symptoms and clinical findings.
- Identifying the Cause of Symptoms: EMG can assist in identifying the underlying cause of symptoms. For example, if a patient complains of muscle weakness, EMG can help determine whether it is due to nerve damage, muscle disease, or another issue.
- Assessment of Recovery: In cases where a patient has undergone treatment or surgery, EMG can be used to assess the progress of recovery. By comparing pre-treatment and post-treatment EMG results, healthcare providers can determine the effectiveness of interventions.
- Documentation for Legal and Insurance Purposes: IMEs often serve as documentation for legal and insurance purposes. EMG results can be included in IME reports to provide objective evidence of a patient’s neuromuscular status, which can be crucial in legal and insurance claims.
- Expert Opinions: EMG results are typically interpreted by specialists, such as neurologists or physiatrists, who can provide expert opinions during IMEs. These specialists can offer insights into the significance of EMG findings in the context of the patient’s overall health and medical history.
It’s important to note that EMGs are just one component of an IME, which typically involves a comprehensive evaluation of a patient’s medical condition, history, and clinical findings. The use of EMGs in IMEs ensures a thorough and objective assessment, particularly in cases involving neuromuscular conditions or injuries.
Why would a doctor order an EMG test?
A doctor may order an electromyography (EMG) test for several reasons. One common reason is to evaluate nerve and muscle function in patients with symptoms such as muscle weakness, numbness, tingling, or pain. By measuring electrical activity in the muscles, an EMG can help identify and diagnose nerve-related conditions such as peripheral neuropathy, carpal tunnel syndrome, or radiculopathy.
Additionally, an EMG can be used to assess the extent and progression of certain neuromuscular disorders, such as muscular dystrophy or amyotrophic lateral sclerosis (ALS). It can provide valuable information about the condition’s severity, help determine treatment options, and monitor the effectiveness of ongoing therapies.
Furthermore, an EMG may be ordered as part of an independent medical examination (IME) when there is a need to assess an individual’s functional capabilities or disability. This evaluation can assist in determining the extent of impairment or disability caused by an injury or medical condition, which may have implications for legal or insurance purposes.
In summary, an EMG test can be ordered by a doctor to evaluate nerve and muscle function, diagnose nerve-related conditions, assess neuromuscular disorders’ severity, and determine functional capabilities or disability for legal or insurance purposes during an independent medical examination.
What diseases can an EMG detect?
Electromyography (EMG) is a diagnostic procedure that evaluates the function of nerves and muscles by measuring the electrical activity produced by them. It can be a valuable tool in helping doctors diagnose a variety of conditions that affect the nervous system and muscles.
An EMG can detect and provide valuable information about conditions such as:
1. Neurological Disorders: EMG can identify abnormalities in nerve function, which can help diagnose conditions such as peripheral neuropathy, radiculopathy, carpal tunnel syndrome, and sciatica. It can also help differentiate between nerve impairments caused by conditions like multiple sclerosis or amyotrophic lateral sclerosis (ALS).
2. Muscle Disorders: EMG can help diagnose muscle disorders such as myopathy, muscular dystrophy, and myasthenia gravis. It can identify muscle weakness, muscle inflammation, or muscle damage, providing insights into the underlying cause and severity of the condition.
3. Nerve Injuries: EMG can assess the extent and location of nerve injuries, such as nerve compression or entrapment, which commonly occur in conditions like herniated discs, pinched nerves, or trauma-related injuries.
4. Nerve Conduction Studies: Combined with EMG, nerve conduction studies can evaluate nerve conduction velocity, which helps identify conditions like nerve damage, demyelinating diseases, or peripheral neuropathy.
However, it’s important to note that an EMG alone cannot provide a definitive diagnosis. Instead, it assists healthcare providers in gathering valuable information to complement clinical findings, medical history, and other diagnostic tests in order to make a comprehensive and accurate diagnosis.
If you suspect that you may have a condition affecting your nerves or muscles, it is essential to consult with a healthcare professional who can evaluate your symptoms and determine whether an EMG is necessary to aid in diagnosis and treatment planning.
How painful is an EMG nerve test?
An EMG nerve test is generally considered to be a minimally invasive procedure, but it can cause some discomfort or mild pain. The level of pain experienced during the test may vary depending on individual pain tolerance and the specific area being tested.
During the EMG test, a small, thin needle electrode is inserted into the muscles being evaluated. This process may cause a brief sharp or stinging sensation. The needle is used to detect and record the electrical activity produced by the muscles during rest and contraction.
While the insertion of the needle may cause some discomfort, the actual recording of the muscle activity should not be painful. Patients may feel a tingling or slight pressure as the electrode is moved around to different muscle areas. The technician conducting the test will communicate with the patient throughout the procedure to ensure their comfort and address any concerns or pain levels they may experience.
It’s important to note that the discomfort experienced during an EMG test is typically temporary and subsides shortly after the procedure is completed. If any pain or discomfort persists or worsens after the test, it is advised to contact your doctor or the medical professional who conducted the test for further guidance.
What happens if EMG is abnormal?
If an electromyography (EMG) test results in an abnormal finding, it could indicate several potential issues related to nerve and muscle function. The specific implications of an abnormal EMG depend on the individual case and the underlying condition being evaluated.
In some cases, an abnormal EMG may suggest nerve damage or dysfunction. This could be caused by conditions such as peripheral neuropathy, radiculopathy (compression or irritation of nerve roots), carpal tunnel syndrome, or other neuropathies. Nerve conduction studies, which are often done in conjunction with EMG tests, can help pinpoint the location and extent of nerve damage.
An abnormal EMG can also indicate muscle problems, such as muscle inflammation (myositis), muscle wasting (atrophy), or muscle weakness. This may be seen in conditions like muscular dystrophy, myasthenia gravis, or other neuromuscular disorders.
It is important to note that an abnormal EMG does not provide a definitive diagnosis on its own. It serves as a valuable tool for healthcare professionals in assessing nerve and muscle function, and it can help guide further diagnostic tests or treatment plans. A patient with an abnormal EMG result may be referred for additional evaluations, such as imaging studies or consultations with specialists, to determine the underlying cause of the abnormal findings.
The interpretation and implications of an abnormal EMG test should be discussed with a healthcare provider who can provide personalized guidance based on the individual’s specific medical history, symptoms, and examination results. They will be able to provide appropriate recommendations for further evaluations and develop a comprehensive treatment plan tailored to the patient’s needs.
EMG test on legs
When it comes to evaluating nerve and muscle function in the legs, an EMG test can be particularly beneficial. This test, known as an Electromyography (EMG), involves detecting and measuring the electrical activity of muscles in the legs.
During an EMG test on the legs, a healthcare provider will insert a needle electrode into specific muscles in order to record the electrical signals produced by the muscle fibers. These signals are then displayed on a machine called an electromyograph, which allows the healthcare provider to evaluate the health and function of the muscles and the nerves that control them.
There are various reasons why a doctor may order an EMG test specifically for the legs. For example, an EMG can be helpful in diagnosing conditions such as peripheral neuropathy or nerve damage in the legs. It can also be used to assess the muscle function in individuals with conditions like muscular dystrophy or ALS (amyotrophic lateral sclerosis).
While an EMG test on the legs is generally considered safe and well-tolerated, some individuals may experience slight discomfort during the procedure. The insertion of the needle electrodes may cause a brief, sharp sensation, similar to a pinprick. However, the discomfort is usually minimal and temporary.
If the results of an EMG test on the legs are abnormal, it could indicate various conditions or issues. These may include nerve compression, such as from a herniated disc or sciatica, muscle disorders, peripheral neuropathy, or even spinal cord injuries. Abnormal results will typically prompt further evaluation and discussion with a healthcare provider to determine the underlying cause and appropriate treatment options.
An EMG test on the legs can provide valuable information about nerve and muscle function in this specific area of the body. It can help doctors diagnose and assess various conditions and guide appropriate treatment plans. If you have concerns or questions about an EMG test on your legs, it is best to consult with a healthcare professional who can provide personalized information and guidance.
Conclusion
This article provides valuable information on the use of electromyography (EMG) in independent medical examinations (IMEs). It covers various aspects related to EMG testing, including its definition, the reasons why a doctor may order it, the diseases it can detect, the potential pain associated with the test, and the implications of abnormal results. Additionally, the article briefly mentions the possibility of conducting an EMG test on the legs. Overall, this article serves as a useful resource for understanding the importance and procedures of using EMGs in IMEs.
Further Considerations
1. Subjectivity in interpreting EMG results: One challenge in conducting Electromyography (EMG) IME is the subjective nature of interpreting the results. Different physicians may have different interpretations of the same EMG findings, leading to potential discrepancies in diagnosis and treatment recommendations.
2. Limited access to experienced providers: Another challenge with EMG IME is the availability of experienced providers who can perform and interpret the tests accurately. As EMG requires specialized training and expertise, it may be difficult to find qualified practitioners, especially in remote or underserved areas.
3. Patient discomfort during the procedure: EMG involves inserting small needles into muscles to measure electrical activity, which can cause discomfort or pain for some patients. This poses a challenge in obtaining accurate results, as patient discomfort may affect muscle activity during the examination.
4. Potential for false-positive or false-negative results: EMG evaluations of nerve and muscle function are not always definitive, and there is a possibility of false-positive or false-negative results. This can lead to misdiagnosis or overlooking underlying conditions, posing a diagnostic challenge for healthcare professionals.
5. Cost implications and insurance coverage: Independent Medical Examinations, including EMG evaluations, can be expensive, and the cost may not always be covered by insurance. This financial barrier can present challenges for patients who require these evaluations but face difficulties in accessing or affording them.
FAQs About Using EMGs in Independent Medical Examinations (IMEs)
1. What is an independent medical examination (IME)?
An IME is an evaluation conducted by a neutral physician or medical professional to assess an individual’s medical condition, often for legal or insurance purposes.
2. How are EMGs used in IMEs?
EMGs can be used in IMEs to evaluate and diagnose nerve and muscle disorders, providing objective evidence of the patient’s condition.
3. What information does an EMG provide during an IME?
EMGs provide valuable information about the integrity and functioning of the nerves, helping in the evaluation of nerve injuries, compression syndromes, neuromuscular diseases, and other conditions.
4. How does an EMG differ from a nerve conduction study (NCS)?
An EMG records the electrical activity of muscles, while an NCS focuses on measuring the electrical impulses along specific nerves. Both tests are often performed together to obtain a comprehensive evaluation of the neuromuscular system.
5. Are EMGs considered a standard part of an IME?
The inclusion of EMGs in an IME may vary based on the specific circumstances and needs of the evaluation. It is up to the evaluating physician to determine whether an EMG is necessary.
6. Are there any risks associated with having an EMG?
EMGs are generally safe; however, there is a minor risk of infection or bleeding at the site of electrode insertion. These risks are rare and can be minimized by following proper sterile techniques.
7. Can EMGs be performed on any part of the body during an IME?
Yes, EMGs can be performed on various muscles or nerve distributions depending on the patient’s symptoms and suspected conditions, including the legs, arms, neck, back, or other relevant areas.
8. How long does an EMG test typically take during an IME?
The duration of an EMG test can vary depending on the specific muscles or nerves being evaluated. Typically, an EMG can take anywhere between 30 minutes to two hours.
9. Are there any preparation requirements for an EMG during an IME?
Depending on the area being tested, you may be asked to avoid applying any creams, lotions, or oils to the skin before the test. Additionally, it’s essential to inform the physician about any medications or blood thinners you may be taking.
10. Can the results of an EMG be used as evidence in legal proceedings?
Yes, the objective findings obtained from an EMG can be used as supporting evidence in legal proceedings, providing valuable insight into the patient’s condition and helping to establish the extent of their injuries.
Glossary of Terms Used in the Article
1. Electromyography (EMG): A test that measures the electrical activity of muscles and nerves.
2. Independent Medical Examination (IME): An evaluation conducted by a neutral physician to assess a person’s medical condition.
3. Nerve test: A diagnostic procedure that evaluates the functioning of nerves in the body.
4. Doctor: A licensed medical professional who may order an EMG test for diagnostic purposes.
5. Diseases: Medical conditions that can be detected or diagnosed through various tests, including an EMG.
6. Abnormal: Deviating from what is considered normal; in the context of an EMG test, it indicates an irregular result.
7. Test: A procedure used to determine the presence or absence of a medical condition.
8. Legs: The lower extremities of the body, often assessed with an EMG test.
9. Painful: Causing physical discomfort or distress.
10. Electrical activity: The flow of electrical signals within muscles and nerves.
11. Muscles: Soft tissues in the body that enable movement.
12. Nerves: The specialized cells that transmit electrical signals throughout the body.
13. Diagnostic: Relating to the identification of a medical condition or disease.
14. Procedure: A series of steps performed to achieve a specific outcome.
15. Functioning: Referring to the normal operation or activity of a body part or system.
16. Evaluation: The process of assessing or examining something to determine its quality or significance.
17. Physician: A medical doctor trained and qualified to diagnose and treat illnesses and conditions.
18. Neutral: Impartial or unbiased; in an IME context, the examiner is neutral and not involved in the patient’s regular medical care.
19. Medical condition: A state of health or illness that requires medical attention or treatment.
20. Diagnostic purposes: The intention of determining the cause or nature of a medical problem or symptom.